Health care service
To overcome the increased challenges created by rising customer orientation, mounting routine work and unpredictable staffing needs,Futuristic Giga Tech Pvt Ltd is successfully serving in the healthcare sector since last few years. The higher aim here is to serve the nation and the health care organizations through the globe.
The customized solutions offered at Futuristic Giga Tech Pvt Ltd range from patient access to collections help in improving the overall revenue cycle system of the clients. We assure to relieve much of your administrative and operational overhead and work towards increasing your profitability. With our years of experience being an offshore supporting vendor for our Healthcare clients at U.S. we analyse claims, every transaction and take all relevant actions to recover the amount due.
We hold presence in the healthcare industry across payers, providers, healthcare services, e-health and government-funded programs which make it easy for us to handle the responsibilities and relieve you of the extra burden.
Our value added Services include:
RCM Service
Billing Service
Collection Service
The customized solutions offered at Futuristic Giga Tech Pvt Ltd range from patient access to collections help in improving the overall revenue cycle system of the clients. We assure to relieve much of your administrative and operational overhead and work towards increasing your profitability. With our years of experience being an offshore supporting vendor for our Healthcare clients at U.S. we analyse claims, every transaction and take all relevant actions to recover the amount due.
We hold presence in the healthcare industry across payers, providers, healthcare services, e-health and government-funded programs which make it easy for us to handle the responsibilities and relieve you of the extra burden.
Our value added Services include:
RCM Service
Billing Service
Collection Service
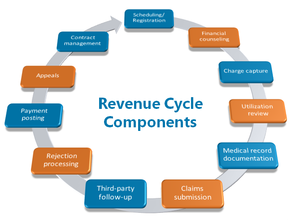
Revenue cycle management service (rcm)
A steady stream of revenue is the desire of one and all be it an independent physician, group practitioner, a billing company or a hospital. But with the growing business, proper management of the revenue related tasks desires a transition. This is possible only when the technology comes into play.Revenue cycle management (RCM) is one such process that manages claims processing, payment and revenue generation via use of technology. This helps keep track of the claims process at every point of its life, so the healthcare provider doing the billing can follow the process and address any issues.
RCM Services offered at Futuristic Giga Tech Pvt Ltd
- Patient Scheduling
- Benefits screening
- Insurance verification
- Pre-Auth and Pre-Certification process
- RAC review and appeals
- End-to-end billing services
- Payment and Denial posting
- Patient Collections
- Late-Stage collections
- Coding Services
- Insurance Follow-ups
- Bad debt recovery
- Health information management
- Denial Management
- Real-time management reporting access to clients
Billing service
Futuristic Gigatech serves various kind of Billing service for health care industry including :
It is the right time for any providers to verify patient’s eligibility, complete pre-authorization process, screen for medical necessity, collect patient responsibility, understand the payment risks then schedule patient for provider visits, etc. At Futuristic Gigatech Pvt Ltd, we clearly understand that this process has to be repeated and meticulously followed for improved cash flow of patient’s up-front collectables like deductibles and copies.
At Futuristic Gigatech Pvt Ltd, our service offers cost-effective and timely patient scheduling services. When a patient calls to make an appointment, a time slot must be scheduled. Likewise at Futuristic Gigatech Pvt Ltd we follow a specific process for patient appointment scheduling for the beneficiary of both the patient and the attendant (MD).
- credentialing
- Pre-registration and Pre-authorization
- Eligibility and Benefit Verification
- Patient Appointment Scheduling Services
- Medical Coding
- Charge Entry
It is the right time for any providers to verify patient’s eligibility, complete pre-authorization process, screen for medical necessity, collect patient responsibility, understand the payment risks then schedule patient for provider visits, etc. At Futuristic Gigatech Pvt Ltd, we clearly understand that this process has to be repeated and meticulously followed for improved cash flow of patient’s up-front collectables like deductibles and copies.
At Futuristic Gigatech Pvt Ltd, our service offers cost-effective and timely patient scheduling services. When a patient calls to make an appointment, a time slot must be scheduled. Likewise at Futuristic Gigatech Pvt Ltd we follow a specific process for patient appointment scheduling for the beneficiary of both the patient and the attendant (MD).
Collection service
Futuristic Gigatech provides collection service for various health care industries . Collection service mainly include the following sub category :
Claims may be electronically submitted to a Medicare Administrative Contractor (MAC) from a provider using a computer with software that meets electronic filing requirements as established by the HIPAA claim standard and by meeting CMS requirements contained in the provider enrollment & certification category area of this web site and the EDI Enrollment page in this section of the web site. Providers that bill institutional claims are also permitted to submit claims electronically via direct data entry (DDE) screens.
Whether you have electronic lock-boxes or receive hundreds (or thousands) of EOB’s mailed weekly to your office, this information must all be posted to a patient’s account in a timely manner. Adjustments or denials must be adjudicated promptly to insure that patients understand their payment responsibilities. Of equal importance is to have the practice’s accounts receivable reflecting the most current payment receipts.
We have organized way of receiving the ERA and the EOB’s from the insurance companies, all the EOBs and ERA’s will be uploaded in our tracking system to be efficiently monitored and used by our expert posting team with absolute precision to reduce the incorrect posting issues.
Charge entry process deals with the entry of details that are needed to get your insurance claims processed. The details i.e., the face sheet of the patient, physician details, information about the insurance coverage of the patient and billing information are entered in this process and hence the claim gets created. It is the most crucial juncture in the billing cycle.
- Electronic and Paper Claim Submission
- Payment Posting
- AR Management
- Denial & Claim Tracking Management
- Patient Collection and Statement Billing
- Revenue Recovery Service
- Impact Analysis
Claims may be electronically submitted to a Medicare Administrative Contractor (MAC) from a provider using a computer with software that meets electronic filing requirements as established by the HIPAA claim standard and by meeting CMS requirements contained in the provider enrollment & certification category area of this web site and the EDI Enrollment page in this section of the web site. Providers that bill institutional claims are also permitted to submit claims electronically via direct data entry (DDE) screens.
Whether you have electronic lock-boxes or receive hundreds (or thousands) of EOB’s mailed weekly to your office, this information must all be posted to a patient’s account in a timely manner. Adjustments or denials must be adjudicated promptly to insure that patients understand their payment responsibilities. Of equal importance is to have the practice’s accounts receivable reflecting the most current payment receipts.
We have organized way of receiving the ERA and the EOB’s from the insurance companies, all the EOBs and ERA’s will be uploaded in our tracking system to be efficiently monitored and used by our expert posting team with absolute precision to reduce the incorrect posting issues.
Charge entry process deals with the entry of details that are needed to get your insurance claims processed. The details i.e., the face sheet of the patient, physician details, information about the insurance coverage of the patient and billing information are entered in this process and hence the claim gets created. It is the most crucial juncture in the billing cycle.